Mubarak Sadiq Abubakar
Russia
Integrating Public Health Initiatives into Clinical Settings to Improve Outcomes for Malnourished Patients in Nigeria, with a focus on preventing NCDs
Abubakar Mubarak Sadiq1, Leen Mutasim Awad Abbas2
1. School of Medicine and Life Sciences, Far Eastern Federal University, Vladivostok, Russia
2. School of Medicine, Grigol Robakidze University, Tbilisi, Georgia
Abstract
Background
Background
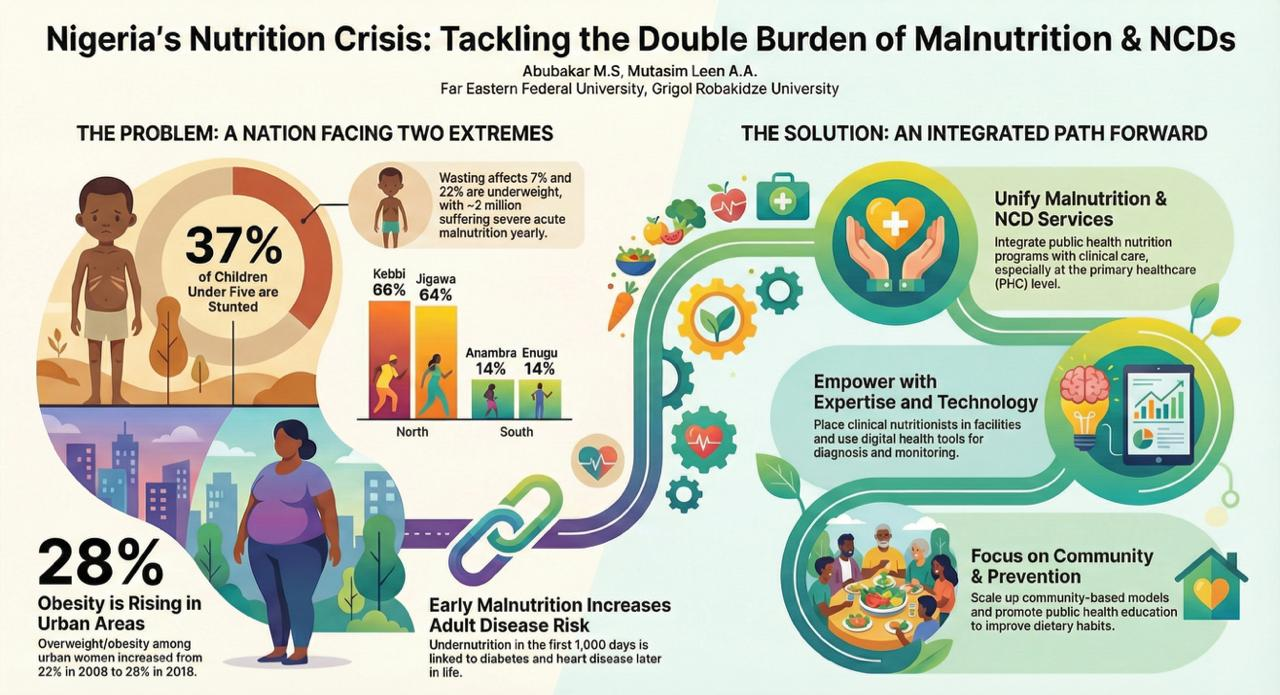
Nigeria is experiencing a nutrition transition, facing the “double burden” of malnutrition—undernutrition and overnutrition—across different demographics [1,2]. Public health nutrition programs operate largely in silos, while clinical management of diet-related diseases lacks upstream integration with prevention efforts [3]. The co-existence of high rates of stunting (37%), wasting (7%), and underweight (22%) among children under five with rising prevalence of obesity and hypertension among adults illustrates the need for unified, multisectoral approaches [4,5].
Methods
Methods
This article employs a desk-based analysis of secondary data from:
• National Demographic and Health Surveys (NDHS)
• WHO/UNICEF databases
• Peer-reviewed journal articles
• Nigerian government health reports
The socio-ecological model and Chronic Care Model (CCM) were used to analyze the interplay between community-based interventions and clinical service delivery. Quantitative trends (2020–2024) were synthesized with policy review and programmatic case studies.
Results
Results
4.1 National Trends
From 2020–2024, protein-energy malnutrition remained high:
• ~2 million children suffered from severe acute malnutrition (SAM) yearly [4,14]
• Wasting: 6.8–7.3%; Underweight: ~20% [14]
4.2 Regional Disparities
• Stunting was most severe in the North-West (up to 66%) [13]
• Overweight and obesity increased in urban women, rising from 22% in 2008 to 28% in 2018 [15]
4.3 Interaction with NCDs
• Low birth weight and childhood undernutrition are linked with adult obesity, diabetes, and cardiovascular disease [6,7,8]
• A study in Ibadan found that poor dietary knowledge contributed to poor disease outcomes among NCD patients [16]
4.4 Integration Models
• mHealth-based training improved PHC worker knowledge on hypertension and diabetes management by 22% [17]
• IMAM’s integration into PHC improved case detection but national treatment coverage remains below 25% [10]
Conclusions
Conclusion
Integrating public health nutrition with clinical NCD care is imperative for Nigeria to mitigate the double burden of malnutrition. Fragmented service delivery and limited clinical nutrition capacity remain major barriers. A coordinated national strategy—grounded in evidence and adapted to regional needs—is needed to shift from reactive treatment to preventive, integrated care.
6. Recommendations
1. Scale community-based PHC models linking NCD and malnutrition services.
2. Institutionalize clinical nutritionists and dietitians in PHC and secondary facilities.
3. Use digital health tools for early diagnosis and monitoring of both malnutrition and NCDs.
4. Promote public health education to improve dietary habits.
5. Improve data systems to track nutrition-related outcomes and program impact.

Leave A Comment