Shikha Pathak
Nepal
Management of Popliteal Artery Injuries: A Case Series of Various Injury Patterns
Satish Vaidya¹, Robin Man Karmacharya¹, Shikha Pathak¹, Swechha Bhatt¹, Aavash Mani Pradhan¹, Jamuna Bhushal¹
¹Department of Surgery, Kathmandu University School of Medical Sciences, Dhulikhel, Nepal
Abstract
Background
The popliteal artery is a continuation of the superficial femoral artery, runs behind the knee, and supplies the lower leg. Popliteal artery injury accounts for 11.1% of peripheral vascular injury. Popliteal artery injuries are rare but limb-threatening, frequently associated with knee dislocations or traumatic lacerations. Delayed recognition can result in severe ischemia, gangrene, or amputation. In resource-limited settings, early diagnosis and individualized surgical management are critical. This case series highlights diverse injury patterns, surgical strategies, and outcomes, providing practical insights for clinicians managing similar vascular injuries.
Methods
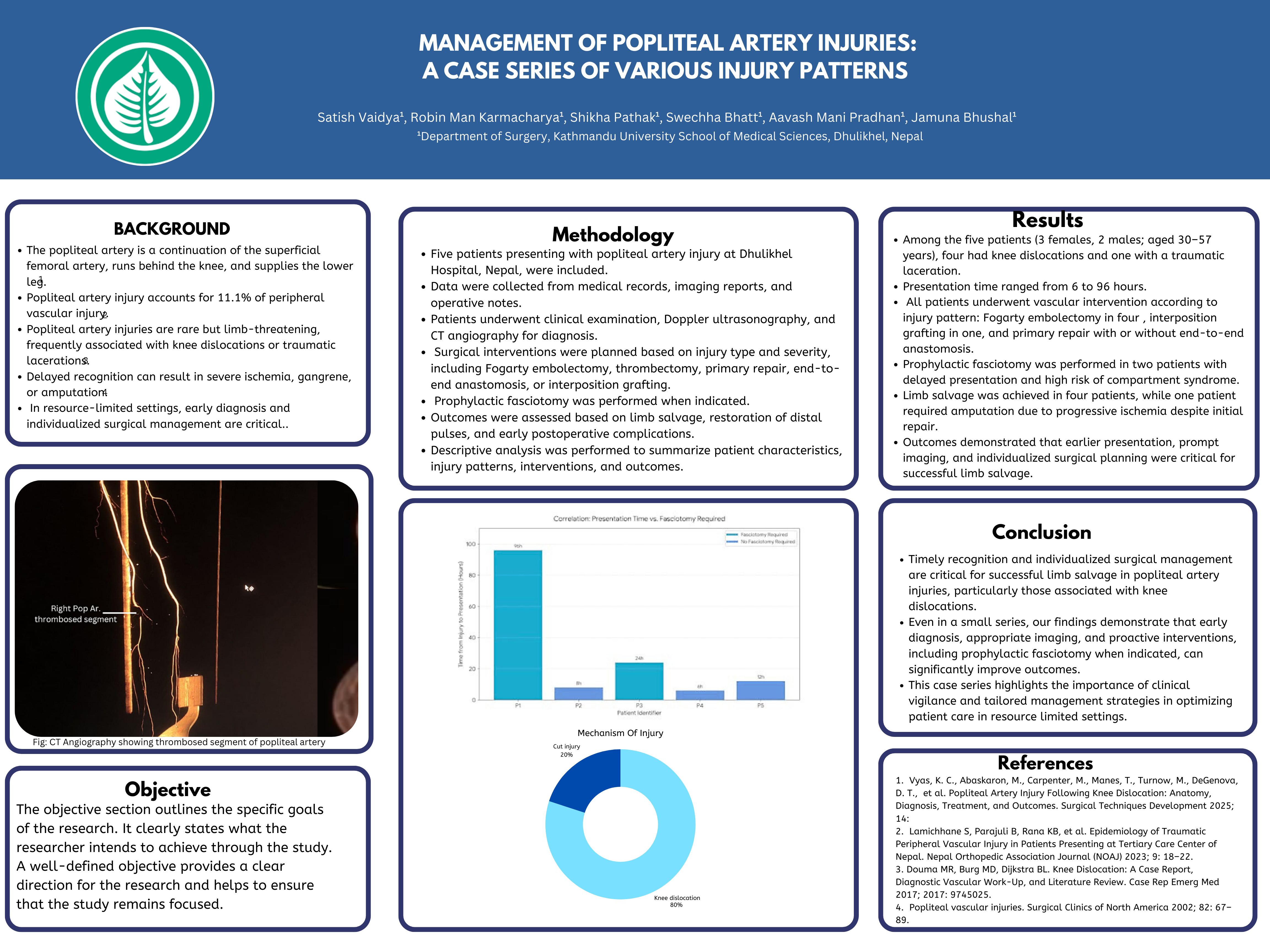
Five patients presenting with popliteal artery injury at Dhulikhel Hospital, Nepal, were included. Data were collected from medical records, imaging reports, and operative notes. Patients underwent clinical examination, Doppler ultrasonography, and CT angiography for diagnosis. Surgical interventions were planned based on injury type and severity, including Fogarty embolectomy, thrombectomy, primary repair, end-to-end anastomosis, or interposition grafting. Prophylactic fasciotomy was performed when indicated. Outcomes were assessed based on limb salvage, restoration of distal pulses, and early postoperative complications. Descriptive analysis was performed to summarize patient characteristics, injury patterns, interventions, and outcomes.
Results
Among the five patients (3 females, 2 males; aged 30–57 years), four had knee dislocations and one with a traumatic laceration. Presentation time ranged from 6 to 96 hours. All patients underwent vascular intervention according to injury pattern: Fogarty embolectomy in four interposition grafting in one, and primary repair with or without end-to-end anastomosis. Prophylactic fasciotomy was performed in two patients with delayed presentation and high risk of compartment syndrome. Limb salvage was achieved in four patients, while one patient required amputation due to progressive ischemia despite initial repair. Outcomes demonstrated that earlier presentation, prompt imaging, and individualized surgical planning were critical for successful limb salvage. This series highlights the variability of popliteal artery injuries and emphasizes the need for rapid diagnosis and tailored surgical management in each case.
Conclusions
Timely recognition and individualized surgical management are critical for successful limb salvage in popliteal artery injuries, particularly those associated with knee dislocations. Even in a small series, our findings demonstrate that early diagnosis, appropriate imaging, and proactive interventions, including prophylactic fasciotomy when indicated, can significantly improve outcomes. This case series underscores the importance of clinical vigilance and tailored management strategies in optimizing patient care in resource limited settings.

Leave A Comment